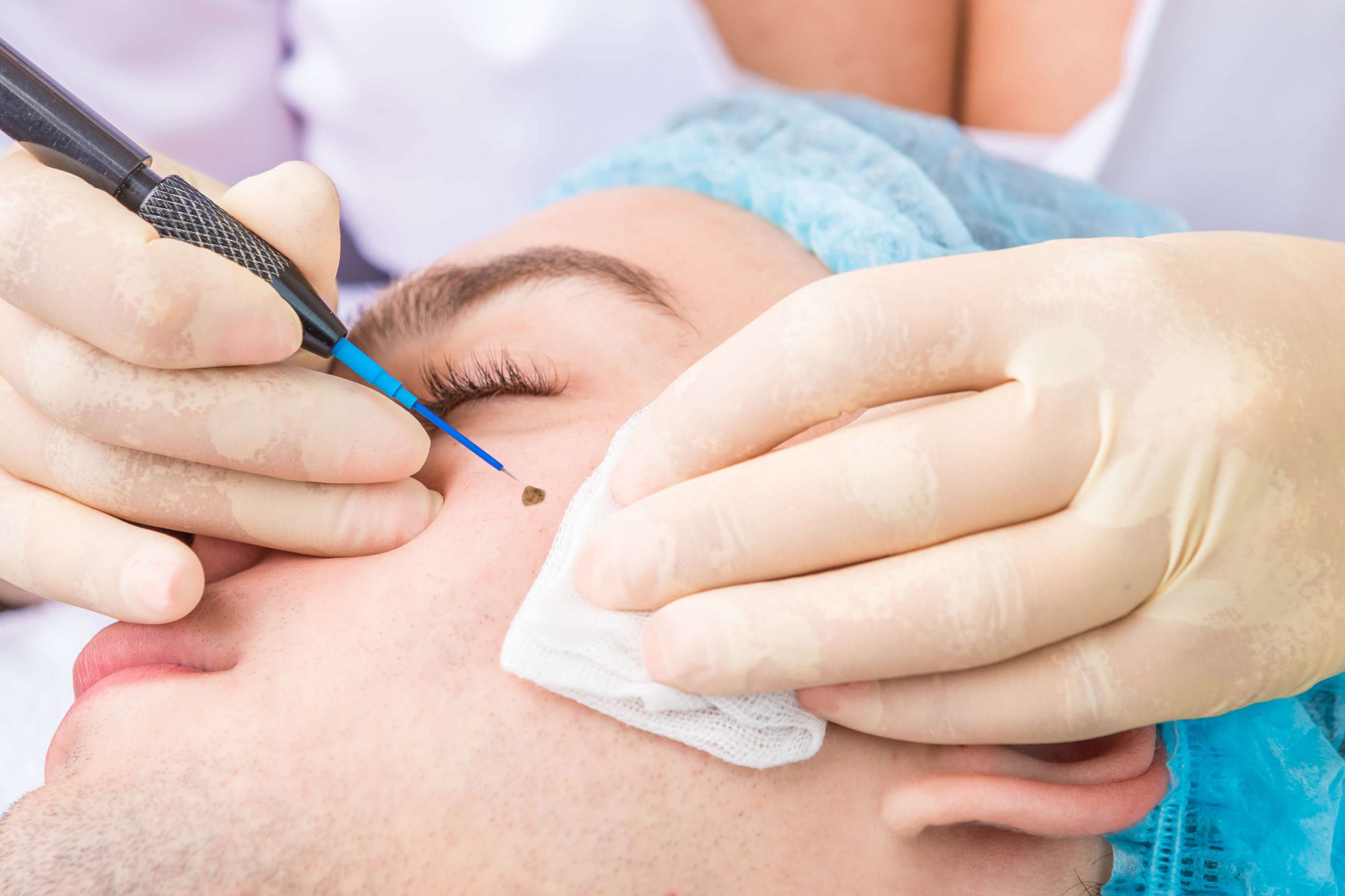
Recently, a young lady with many moles came to me for a second opinion. She has had her mole checked as well as laser mole removal done by another doctor. However, her mole specimens which were sent for laboratory analysis were reported to be too tiny, charred and inadequate for proper evaluation for the exclusion of skin cancer. Understandably, she was anxious!
After clinical consultation and examination, I concluded that her risk for skin cancer was low and all her remaining moles were normal looking. All her moles could have been removed without the need to send specimens for laboratory analysis. I then assured her that it was likely that the moles removed earlier were also normal too. With that assurance, she left the clinic happy and in peace.
Moles are common and generally not attractive. Most people would like to have them removed. In Singapore, this treatment is performed by a myriad of people, accredited skin specialist, beauticians in beauty salons and even some uncles at the night bazaar stall. Very often, people expect mole removal to be risk-free and they do not consider it necessary to have it examined or removed by a skin specialist. They assume that the skin will heal perfectly.
Many people are not aware that scars, indentations and colour changes may occur after mole removal procedures. The moles can also recur when there is incomplete removal. The worst-case scenario is when a cancerous mole was removed unknowingly and incompletely. That would have been disastrous and that was why the patient above was anxious!
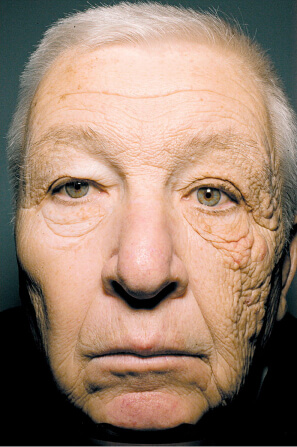
When a patient comes for mole removal. I will evaluate their risk factors: skin type, past histories of skin cancer in the patient and family, history of occupational and recreational sun exposure and etc. If they are assessed to be of low risk, then I will remove their normal looking moles upon request. There is no need for any laboratory analysis. But if they are assessed to be of moderate or high risk, I will surgically remove the suspicious moles and send them for laboratory testing. It is important to be prudent and careful even with simple procedures like mole removal.